Cancer patients searching for “juicer recipes for cancer patients” online face a dangerous reality: most recipes lack critical safety protocols for immunocompromised individuals. When undergoing chemotherapy or radiation, even a simple green juice can introduce life-threatening bacterial risks or interfere with treatment efficacy. Unlike general wellness juicing, cancer-specific formulations require precise ingredient combinations that won’t compromise fragile immune systems or interact with medications. Without clinical oversight, well-intentioned juicing attempts could land patients in the hospital with infections or reduced treatment effectiveness—especially when white blood cell counts are critically low.
The urgency for verified resources becomes clear when considering that 60-80% of cancer patients experience malnutrition during treatment, often turning to juicing for nutrient absorption. Yet standard recipes frequently include contraindicated ingredients like raw kale (high in vitamin K that interferes with blood thinners) or unpasteurized citrus (risking fungal infections in neutropenic patients). This article cuts through the misinformation by outlining the seven non-negotiable elements any legitimate juicing resource must provide for cancer patients—based on medical nutrition standards. You’ll learn exactly how to evaluate recipes for safety, recognize red flags, and partner with your oncology team to integrate juicing without compromising your treatment plan.
The Hidden Dangers of Unverified Juicing During Active Treatment
Cancer treatments create unique physiological vulnerabilities that turn ordinary juicing into a potential hazard. Chemotherapy-induced neutropenia leaves patients with dangerously low white blood cell counts, making raw produce a vector for pathogens like E. coli or listeria. Radiation therapy to the digestive tract can trigger severe mucositis, where acidic juices cause excruciating mouth sores. Most concerning are ingredient-treatment interactions: cruciferous vegetables may accelerate metabolism of certain chemo drugs, while high-antioxidant juices could theoretically protect cancer cells during radiation. Without explicit contraindication warnings, patients unknowingly risk treatment delays or hospitalizations.
Why “Healthy” Ingredients Become High-Risk
Citrus fruits during neutropenia: Oranges and lemons harbor bacteria in their peels that transfer to juice during processing. For patients with absolute neutrophil counts below 500, this creates sepsis risks.
Raw leafy greens: Spinach and kale contain soil-borne pathogens that standard washing won’t eliminate—especially dangerous when mucosal barriers are compromised.
High-fiber produce: Beets and carrots may seem nutritious but can trigger bowel obstructions in patients with gastrointestinal cancers or post-surgery adhesions.
Critical Safety Thresholds You Must Verify
Before trying any recipe, confirm these non-negotiables:
– Absolute neutropenia protocols: Recipes must specify pasteurization methods (like flash-heating to 165°F for 15 seconds) when ANC <1,000
– Mucositis modifications: pH levels above 4.5 to prevent tissue damage (avoid lemon/lime without medical approval)
– Drug interaction flags: Clear warnings for patients on blood thinners (vitamin K sources) or tyrosine kinase inhibitors (grapefruit)
7 Non-Negotiable Elements of Safe Cancer Patient Juicing Resources
Precise Ingredient Measurements with Medical Context
Legitimate resources specify exact quantities like “½ cup peeled, cooked beets (not raw)” instead of vague terms like “a handful.” Each recipe must include:
– Weight-based measurements (grams, not cups) for calorie/nutrient accuracy
– Preparation mandates (e.g., “peel all produce” to remove surface pathogens)
– Treatment-phase indicators (safe only during remission vs. active treatment)
Red flag: Recipes listing “1 apple” without variety specification—Gala apples have 3x more sugar than Granny Smiths, impacting blood glucose in diabetic patients.
Complete Nutritional Breakdowns Per Ounce
Effective resources provide lab-verified nutrient profiles including:
– Calories per 2oz serving (critical for patients with appetite loss)
– Key electrolyte levels (sodium/potassium for those with vomiting-induced imbalances)
– Antioxidant concentrations (measured in ORAC units to prevent interference with radiation)
Example: A safe post-chemo recipe might show 45 kcal/2oz, 120mg potassium, and <500 ORAC units to avoid radiation shielding.
Ingredient-Specific Therapeutic Rationale
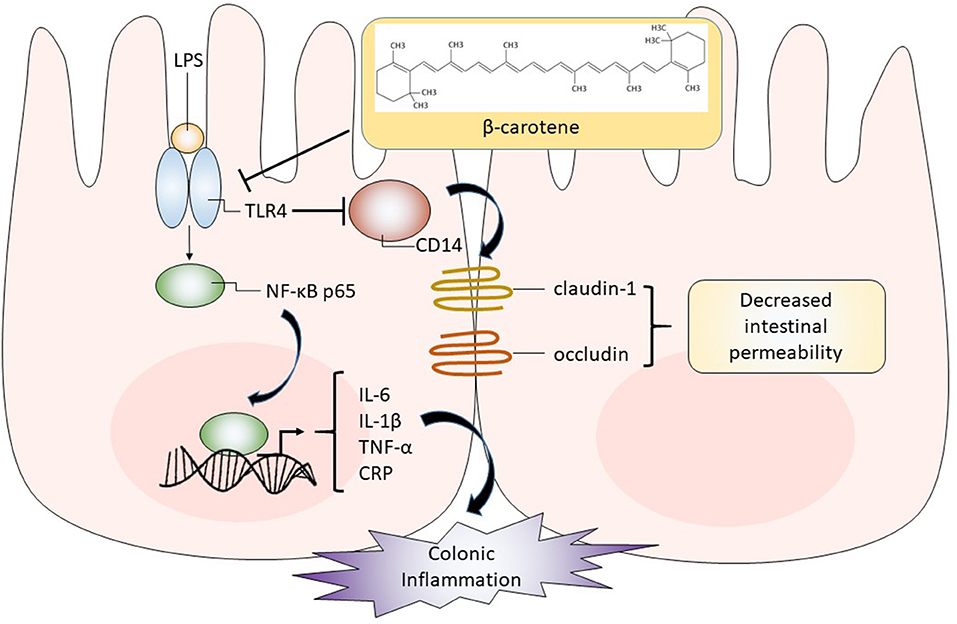
Every component must justify its inclusion with clinical purpose:
“Carrot (½ cup, cooked): Provides 107% daily vitamin A as beta-carotene to support mucosal healing without exceeding safe limits for lung cancer patients on retinoid therapy.”
Avoid resources claiming “boosts immunity” without specifying mechanisms—this oversimplification ignores how treatments deliberately suppress immune activity.
Specialized Preparation Safety Protocols
Verified resources mandate:
1. Produce selection: Only firm, blemish-free items (soft spots harbor bacteria)
2. Surface decontamination: 3-minute soak in 3% hydrogen peroxide solution before peeling
3. Equipment sanitation: Juicer parts boiled for 10+ minutes pre-use (not just rinsed)
4. Immediate consumption: Zero storage recommendations—freshly made juice only
Critical note: Never use “cold-pressed” claims as safety guarantees—high-pressure processing (HPP) is required to eliminate pathogens, which home juicers can’t achieve.
Clinical Evidence Supporting Ingredient Choices
Credible resources cite studies like:
– “Ginger root (1 tsp grated) reduced chemotherapy-induced nausea by 40% in JCO 2013 trial (N=576)”
– “Blueberry anthocyanins increased cisplatin efficacy in ovarian cancer models (Cancer Research 2020)”
Avoid anecdotal claims like “cleanses toxins”—oncology has no clinical definition for this term.
Treatment-Specific Contraindication Warnings
Essential alerts must include:
| Treatment Type | Forbidden Ingredients | Physiological Risk |
|———————|—————————–|—————————–|
| Radiation (Head/Neck)| Citrus, tomatoes | Exacerbates mucositis pain |
| Blood Thinners | Kale, spinach, parsley | Vitamin K reduces drug efficacy |
| Tyrosine Inhibitors | Grapefruit, starfruit | Alters drug metabolism |
Practical Daily Implementation Guidance
Effective resources provide:
– Optimal timing: “Consume 2 hours before chemo to avoid nausea triggers”
– Portion progression: Start with 1oz servings, increasing only if no diarrhea occurs
– Symptom response protocol: “Discontinue beet juice if urine turns pink (indicates kidney strain)”
Evaluating Juicing Resources with Your Oncology Team
Bring this checklist to your next appointment:
1. Verify medical oversight: Does the resource list an oncology dietitian on its advisory board?
2. Cross-check contraindications: Ask your pharmacist to screen ingredients against current medications.
3. Request lab testing: Hospitals can analyze homemade juice for pH levels and bacterial counts.
Pro tip: Print the recipe’s ingredient list and ask: “Could this interact with my [specific treatment] on [specific day] of my cycle?” Timing matters—some ingredients are safe during recovery weeks but dangerous during infusion days.
When to Avoid Juicing Altogether
Immediate cessation is required if you experience:
– Fever >100.4°F (potential bacterial infection from produce)
– Severe diarrhea (indicates possible C. diff overgrowth)
– Blood in stool (high-fiber juices can aggravate GI tumors)
During active neutropenia (ANC <500), switch to medically formulated oral nutritional supplements until counts recover. Your care team may approve juicing only when:
– Absolute neutrophil count >1,500 for 48+ hours
– No active mucositis ulcers
– No ongoing antibiotic treatment
Final Note: Safe juicing for cancer patients isn’t about trendy recipes—it’s medical nutrition therapy requiring oncology oversight. Never prioritize internet suggestions over your treatment team’s guidance. If a resource lacks all seven critical elements outlined here, treat it as potentially hazardous. Request a referral to a board-certified oncology dietitian who can develop personalized juicing protocols aligned with your treatment phase and lab values. Remember: during active therapy, “natural” doesn’t equal safe—your life depends on evidence-based precision. For verified resources, consult the Academy of Nutrition and Dietetics’ Oncology Nutrition Database or ask your hospital’s nutrition department for institutionally approved protocols.





